Chiari Malformation Testing & Diagnosis
The diagnostic process begins with a complete medical history and physical examination. These are followed by a complete neurological evaluation that will assess your specific symptoms and neurological function. The patient with a Chiari malformation may have an entirely normal examination. In such cases, it becomes more difficult to determine if the Chiari is indeed a problem and if surgery is indeed the best solution. In such cases, judgment of an experienced neurosurgeon becomes very important. When the neurological examination is abnormal, the pattern of abnormal findings can make it easy to pinpoint the problem to the cervical spinal cord and brainstem.
Patients may have difficulty with coordination, balance, eye movement, sensation, and strength. The reflexes may be too active or not active enough. Other reflexes that are never present except when the spinal cord is not functioning normally—pathological reflexes—may also be detected.
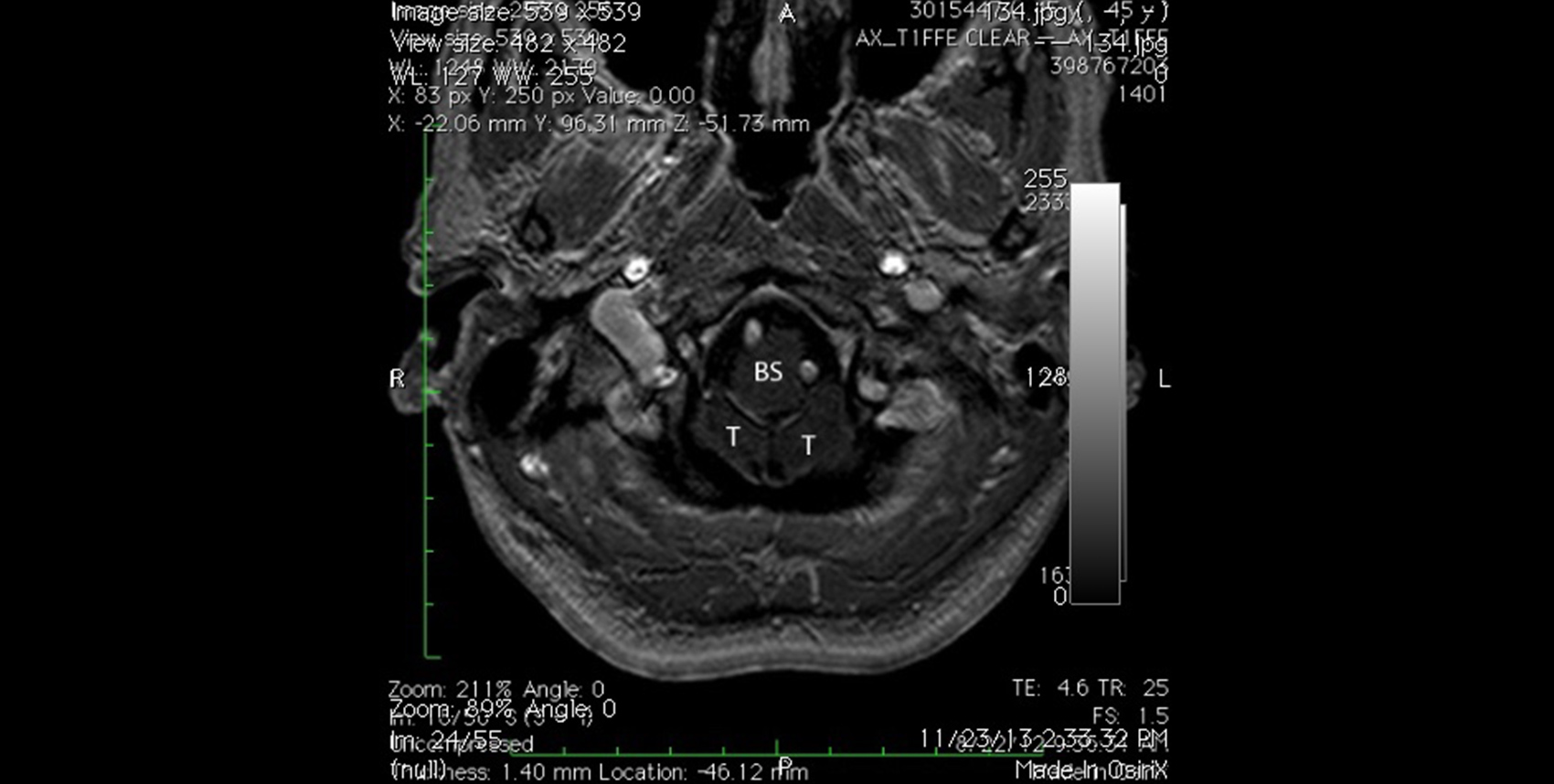
Magnetic resonance imaging (MRI) is the best diagnostic tool for detecting Chiari malformation. This test provides the doctor with detailed anatomical information regarding the structure of the base of the brain. The criteria for diagnosing Chiari malformation, however, are very arbitrary. As a result, some doctors adhere to a rigid standard—5 mm of tonsillar herniation—before making the diagnosis of Chiari, even in the face of typical patient symptoms and obvious neurological findings. Hence, many patients with Chiari go undiagnosed and untreated for years. We have developed some MRI imaging strategies that demonstrate the critical problem—brainstem compression—more clearly. These MRI techniques allow us to identify some Chiari patients who would otherwise go undiagnosed.
What happens if your symptoms reoccur?
Some patients may undergo Chiari surgery by another surgeon and either fail to experience any improvement in symptoms or, worse, they may deteriorate. This is considered failed Chiari surgery. Perhaps 20% of patients that I have treated have been treated elsewhere with poor results. There are several possible explanations:
- Excessive bone removal causing slumping or further settling of the cerebellar tonsils and causing the Chiari problem to recur after initial improvement.
- Failure to do a dural patch, resulting in inadequate decompression of the brainstem.
- Failure to perform intradural exploration, leaving compression of the brainstem unresolved.
- CSF leak with pseudomeningocele formation which results in headache, dizziness, nausea whenever the patient is upright. In addition, the CSF leakage can promote further settling of the brain and recurrence of the Chiari malformation.
- Failure to recognize cervical stenosis, which can mimic all the symptoms of the Chiari malformation.
- Failure to recognize and treat lumbar tethered spinal cord, which occurs in 20% of patients with Chiari.
All these problems can be corrected. The patient can go on to have an excellent result.
If you are a new patient, please contact us.